Revenue Cycle Management
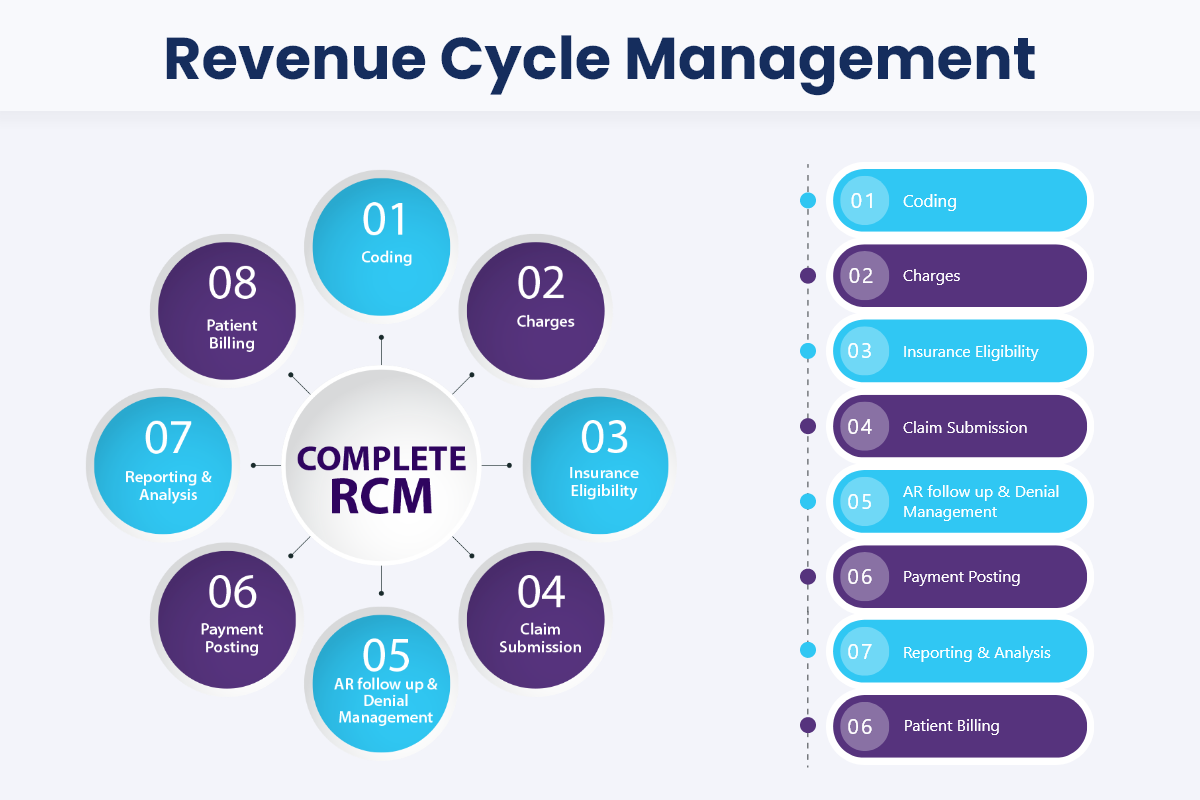
Revenue Cycle Management (RCM) refers to the process of identifying, collecting, and managing the practice’s revenue from payers based on the services provided. A successful RCM process is essential for a healthcare practice to maintain financial viability and continue to provide quality care for its patients. This is the right time to engage with a partner who brings deep and clear understanding of the Revenue Cycle Management. We at Indus Medica manage your billing, coding and claim submissions, so you can focus on patient care.
Billing
We understand the Importance of clean claim submission. Therefore, our billing department ensures that all bills are submitted with the correct & required information to avoid delays & denials. Our trained staff will audit & make sure the information related to patient demographics, CPT & ICD codes along with modifiers, number of units, and date of service are entered before submitting the claim. Therefore, we help you in efficiently managing your cash flow.
Coding
Medical coding can be a critical process in which the covered patient’s history, diagnosis, prescription and procedures are transmitted into medical codes. Effective medical billing and coding in-house is tough, and is best achieved when outsourced to professional medical coders. Outsourcing your medical coding services to Indus helps you to optimize your revenue while reducing compliance risks. We are experts in Pain Management medical billing and coding.
Account Receivable
It has been observed that revenues for most clinics are stuck in this stage where Insurance Follow up is not a priority. Thousands of dollars are waiting to be collected but follow up with long hold periods on the phone with Insurance companies is tedious and must be minimized with timely followups . Our Account Receivable’s are well versed in identifying patient accounts that require follow-up and take the necessary action to collect unpaid and partially paid claims.
Denial Management & Appeals
The process of Denial Management has only one key – ANALYSIS, once the root cause of denial is figured, correcting it and getting paid for it is not a task. The skill of a specialist is required to get the perfect analysis into a claim. It is one of the biggest nightmares for a healthcare organization. Most of the time, the main reason for denial is incorrect or missing data. We ensure sure that we chart every code according to the denial type and responsibility. To arrive at a perfect denial resolution and our Agent’s are expert in Denial Management.
Patient Collections Services
To ensure your patients remain happy, and your office meets its financial goals you need you need a medical collections company that cares about the patient experience and delivers superior performance. Your patient will receive a positive service from our trained Patient Financial Advocates who are experts in healthcare billing collections.

